
by Joe Mehall - Wednesday, July 1, 2020

Yesterday, I spent the day with my wife and sons and visited my mother. It was a perfect Father’s Day except that my dad wasn’t there. He passed away in December 2006. Earlier that year he had a long battle with Lyme disease. Initially I thought he won that battle, but instead it contributed to his demise.
Today is my sister’s wedding anniversary. I was proud to walk Karen down the aisle, but it should have been Dad. She contracted Lyme disease earlier in the 1990s. That’s two out of four members of my childhood family. A longtime NRA employee, Karen shared her story in the NRA’s official journals, hoping to make hunters and other outdoor enthusiasts more aware of the signs.
In the years since, a close family friend found out he had Lyme disease, which temporarily paralyzed his face, a condition known as Bells palsy. Another friend tested positive for it last year, and I know someone else who thinks he has it now. Nearly every time I go outside, I find another tick crawling on my leg or arm. I’ve probably found well over two dozen ticks on me so far this year while just doing very basic things in my yard. My family and I automatically check for ticks after spending any time outdoors.

Ticks don’t social-distance—in pandemics or otherwise—so know how to prevent Lyme disease and recognize its symptoms. Especially as we head outdoors for the July 4th holiday week, those family picnics, cookouts and camping and fishing trips make us easy targets. Early detection of the disease can make all the difference in the world, so be sure to monitor any areas where you have recently removed a tick.
How the Disease Is Transmitted
Lyme disease is the most common tick-bourne illness in America. It comes from the bite of a deer tick. This tick is no bigger than the size of a pinhead, carrying the bacterium Borrelia burgdorferi that it picked up from another host. Borrelia burgdorferi is named after scientist Wilhelm "Willy" Burgdorfer, who first isolated the bacterium in 1982, and it’s called Lyme disease because it was first documented in Lyme, Conn.

I was young when Lyme disease first hit the news, but I remember thinking it was probably not going to happen to anyone I knew. I was wrong. Growing up in southern Maryland meant ticks were a part of life. Playing in the back yard or building a fort in the woods often ended with finding a tick on some part of the body. Nearly 100,000 cases in 48 states were on file with the Centers for Disease Control and Prevention from 1982-1996. My sister was one of those cases in 1996. While hunters obviously are at risk, so is everyone who is actively doing things outdoors. If you’ve just taken your dog for a walk, gone golfing or cut the grass, you may find a tick on your body or clothes.

Prevention Tips
Lyme disease experts suggest wearing light-colored, long-sleeved shirts and pants when possible to make ticks easier to spot. Try tucking your shirt into your pants and your pant legs into your shoes or boots (if possible) to keep ticks from getting under your clothing. Wear a hat and pull long hair back. Use insect repellents with DEET on your clothing and skin, which also helps to keep away mosquitos and other flying insects. Ticks can’t jump, but they live in shrubs, bushes and tall grasses and crawl or drop onto us as we pass by them. When you go back indoors, check yourself and others for ticks, especially the areas like your scalp and back that are tough to see. Also check your pets. Ticks often hitchhike on your dog and end up crawling around in the house in search of a host. I’ve personally seen ticks on our dog a few times this year.
If You Find a Suspected Tick Bite
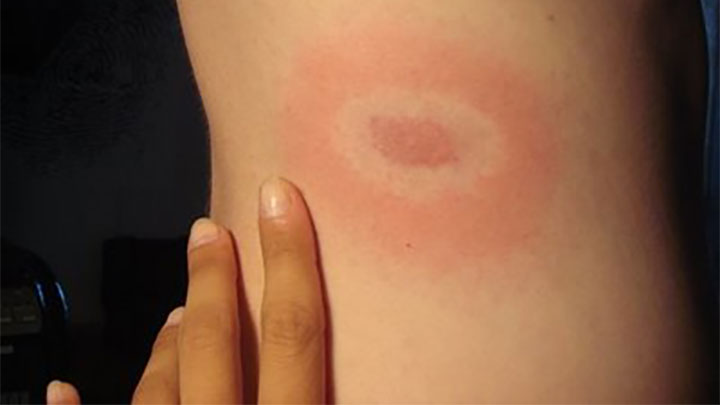
Remember two things: Not every tick bite itches and not every tick bite causes a rash, often in the form of a signature “bullseye” ring around the bite site. So if you have a tick embedded or got bitten, you might not know it. A bite on the back of your neck that doesn’t itch won’t get your attention. If you do get itchy or notice you have skin irritation, look for a rash or tick bite.
If You Find an Embedded Tick
If you live in or visit certain areas known to be polluted with ticks, you or someone you know eventually will find one attached. Use tweezers, which make it easier to grip the tick’s body. Get as close as possible to the tick’s mouth and pull the tick straight back. Don’t flatten it, twist it or take a match to it because you might tear the tick in half, leaving part of it under your skin. Just as bad, this could make the tick regurgitate infected fluids into your bloodstream. Smothering it with alcohol won’t work either because these parasites store enough oxygen to keep feeding on your blood.
Once the tick is removed, disinfect the bite site. Put it in a jar or other container so you have it for testing if you develop Lyme disease symptoms later.
Do You Have Any of These Symptoms?
Karen went to the doctor three or four times in a six-week period. She thought she had the flu. She had no energy but could not point to a specific cause. She had a low-grade fever, headache, painful joints and a sore throat with swollen lymph nodes. She had blood tests, but nothing showed. She worried that by the time doctors learned what was wrong, the health issue would be even more advanced. Twenty-plus years ago not only was Lyme disease not as prevalent, but as she wrote about in American Hunter and American Rifleman, Lyme disease symptoms mimic other health problems, which can make Lyme very difficult to diagnose. You may think that headache is coming from dehydration oarly symptoms of Lyme diseaser that any fatigue is because you’re busier at work. That tired, rundown feeling can be a sign of trying to fight off the flu or of not sleeping well. And if you have arthritis, that joint pain is no surprise. However, the CDC has long documented that these are early symptoms of Lyme disease.
In addition to the above symptoms that start typically three to 30 days after the tick bite, there is that telltale “bullseye” rash I mentioned that the CDC says is present in 70 to 80 percent of cases. Those who get it say it sometimes feels warm to the touch and often clears up as it enlarges, which is what creates that bullseye appearance.
However, like my father, some people who contract Lyme disease have it for many months before it is diagnosed. LymeDisease.org, a website dedicated to Lyme disease advocacy, education and research, explains that if the disease is not diagnosed and treated early, it may become late-stage or chronic. At this point, symptoms escalate and can include: severe headaches and neck stiffness as the disease spreads through the nervous system; dizziness; shortness of breath; debilitating fatigue; nausea; diarrhea; low-grade fever; intermittent pain in tendons, muscles, joints and bones; nerve pain; numbness or tingling in the hands and feet; pain in larger joints such as the knees; facial palsy, or drooping of a side of the face; and heart palpitations or a slow, irregular heartbeat. This last symptom, known as Lyme carditis, only occurs in a few cases out of every 100 as Lyme disease bacteria enters heart tissues and impedes electrical signals from the upper to lower heart chambers. Visit the LymeDisease.org website for more information on symptoms and review its online publication, the Lyme Times, for more topics related to the disease.
Treatment
As I learned from my family’s experience, you need a blood test to diagnose Lyme disease. If you test positive for it but are not sure how long you have had it, other tests can determine how long you’ve been infected. Fortunately, Lyme disease can be treated with antibiotics because it is a bacterial disease. If you catch it in the early stages, oral antibiotics are said to work in 95 percent of cases. My dad had late-stage Lyme disease and had to have multiple courses of intravenous antibiotics. How long you’ve had it also determines the type and extent of treatment you receive. In the most severe cases, doctors only can treat symptoms as they arise.
Fortunately, while we hunters and other outdoorsmen know to check for ticks, most ticks do not carry Lyme disease. Like a mosquito bite, every tick bite causes a bump and/or redness. This doesn’t mean you have Lyme disease and usually goes away within a few days.
Resources
Fortunately, there is considerable information out there on Lyme disease as medical professionals and sportsmen’s organizations continue to promote public awareness. As an NRA Life member, for example, I know how the NRA looks out for hunters through programs, services and lobbying efforts to protect our freedoms. Just one of those services is a series of books and other materials called the NRA Hunter’s Educational Series, including a “Lyme Disease” brochure. In addition, this NRA website and NRA’s American Hunter keep close tabs on the disease for us hunters.
Do yourself a favor and visit one of the sources mentioned in this article for more information. As deer ticks continue to increase their geographical spread, if you start experiencing flu symptoms, never discount that it might be due to a tick bite.
About the Author
Joe Mehall grew up in LaPlata, Md., with his sister, Karen Mehall Phillips, director of communications for the NRA Hunters’ Leadership Forum and senior editor for NRA Publications. He lives in Maryland with his wife, Tricia, and their sons, Andrew and Joey, and beagle, Rigby. Joe enjoys sharing his love of hunting, fishing, coaching and playing sports—and he always checks for ticks.
E-mail your comments/questions about this site to:
[email protected]
Proudly supported by The NRA Foundation and Friends of NRA fundraising.
